Therapeutic Vaccines: Why Have They Succeeded in Some Diseases and Failed in Others?
Keywords:
Vaccines, Therapeutic, Immunotherapy, Antigens, Neoplasm Immune Tolerance, T-Lymphocyte Exhaustion, Tumor Microenvironment, BiomarkerAbstract
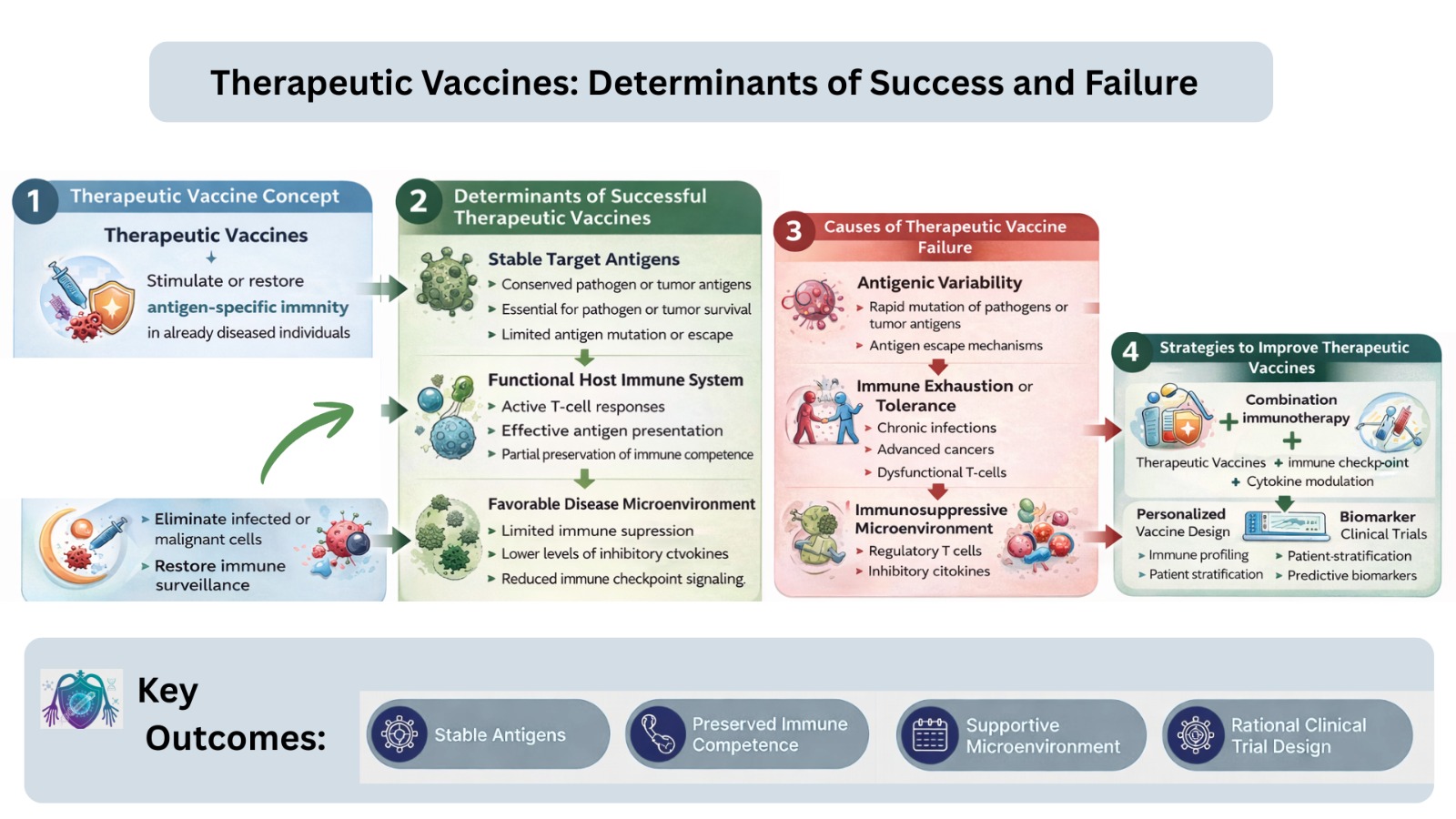
Therapeutic vaccines generate or restore antigen-specific immunity, providing a unique clinical approach as compared to prophylactic vaccination. Although therapeutic vaccines have intermittent efficacy in different diseases, their optimistic response is reported in some infectious diseases whereas, insignificant efficacy in many chronic and immune-dysregulated malignancies. This questions the underlying biological and translational determinants and seek scientific explanations for these divergent outcomes. Therapeutic vaccines have been linked with well-characterized conserved target antigens, partially preserved immune competence, and disease settings that allow effective immune activation., which predetermines the success of therapeutic vaccines. In contrast, failure of these vaccines is often associated with antigenic variability, immune exhaustion or tolerance, prevailing immunosuppressive mechanisms, and recalcitrant disease microenvironments that impair effective immune interactions. Additional complications include vaccine platforms, poor adjuvants as well as concerns related to design of clinical trials like poor endpoints and poor patient stratification. Immunology, biomolecular profiling and vaccine engineering technologies have elucidated these challenges and identified ways of overcoming them. The translational efficacy can be improved by integrating therapeutic vaccines with immune-modulating factors, selection of targeted antigens, and the use of biomarkers to guide the clinical process. It is essential to define success and failure to guide the development of next-generation therapeutic vaccines rationally.
References
1. Tian Y, Hu D, Li Y, Yang L. Development of therapeutic vaccines for the treatment of diseases. Mol Biomed. 2022;3(1):40. https://doi.org/10.1186/s43556-022-00098-9
2. Li J, Ross JL, Hambardzumyan D, Brat DJ. Immunopathology of glioblastoma. Annu Rev Pathol. 2026;21(1):135-162. https://doi.org/10.1146/annurev-pathmechdis-042524-025950
3. Singha SP, Memon S, Bano U, Isaac AD, Shahani MY. Evaluation of p21 expression and related autism-like behavior in Bisphenol-A exposed offspring of Wistar albino rats. Birth Defects Res. 2022;114(11):536–50. https://doi.org/10.1002/bdr2.2022
4. Weerarathna IN, Doelakeh ES, Kiwanuka L, Kumar P, Arora S. Prophylactic and therapeutic vaccine development: advancements and challenges. Mol Biomed. 2024;5(1):57. https://doi.org/10.1186/s43556-024-00222-x
5. Maier JA, Castiglioni S, Petrelli A, Cannatelli R, Ferretti F, Pellegrino G, et al. Immune-mediated inflammatory diseases and cancer: a dangerous liaison. Front Immunol. 2024;15:1436581. https://doi.org/10.3389/fimmu.2024.1436581
6. Bano U, Memon S, Shahani MY, Shaikh P, Gul S. Epigenetic effects of in utero bisphenol A administration: Diabetogenic and atherogenic changes in mice offspring. Iran J Basic Med Sci. 2019;22(5):521–8. https://doi.org/10.22038/ijbms.2019.29909.7357
7. Memon S, Bano U, Shahani MY. Maternal exposure to Bisphenol-A induces epigenetic changes in metabolic syndrome markers of offspring. FASEB J. 2018;32(Suppl 1):774–2. https://doi.org/10.1096/fasebj.2018.32.1_supplement.774.2
8. Carabelli AM, Peacock TP, Thorne LG, Harvey WT, Hughes J, Peacock SJ, et al. SARS-CoV-2 variant biology: immune escape, transmission and fitness. Nat Rev Microbiol. 2023;21(3):162-177. https://doi.org/10.1038/s41579-022-00841-7
9. Baharom F, Hermans D, Delamarre L, Seder RA. Vax-Innate: improving therapeutic cancer vaccines by modulating T cells and the tumour microenvironment. Nat Rev Immunol. 2025;25(3):195-211. https://doi.org/10.1038/s41577-024-01091-9
10. Corrado M, Pearce EL. Targeting memory T cell metabolism to improve immunity. J Clin Invest. 2022;132(1). https://doi.org/10.1172/JCI148546
11. Bretscher PA. The problem of host and pathogen genetic variability for developing strategies of universally efficacious vaccination against and personalised immunotherapy of tuberculosis: potential solutions? Int J Mol Sci. 2023;24(3):1887. https://doi.org/10.3390/ijms24031887
12. Tufail M, Jiang CH, Li N. Immune evasion in cancer: mechanisms and cutting-edge therapeutic approaches. Signal Transduct Target Ther. 2025;10(1):227. https://doi.org/10.1038/s41392-025-02280-1
13. Butterfield LH, Najjar YG. Immunotherapy combination approaches: mechanisms, biomarkers and clinical observations. Nat Rev Immunol. 2024;24(6):399-416. https://doi.org/10.1038/s41577-023-00973-8
14. Waugh S, Cameron CE. Syphilis vaccine development: aligning vaccine design with manufacturing requirements. Hum Vaccin Immunother. 2024;20(1):2399915. https://doi.org/10.1080/21645515.2024.2399915
15. Kaczmarek M, Poznańska J, Fechner F, Michalska N, Paszkowska S, Napierała A, et al. Cancer vaccine therapeutics: limitations and effectiveness—a literature review. Cells. 2023;12(17):2159. https://doi.org/10.3390/cells12172159
16. Wang S, Liang B, Wang W, Li L, Feng N, Zhao Y, et al. Viral vectored vaccines: design, development, preventive and therapeutic applications in human diseases. Signal Transduct Target Ther. 2023;8(1):149. https://doi.org/10.1038/s41392-023-01408-5
17. Gomase VS, Sharma R, Dhamane SP. Immunoinformatics approach for optimization of targeted vaccine design: new paradigm in clinical trials and healthcare management. Rev Recent Clin Trials. 2025;Jul 16. https://doi.org/10.2174/0115748871374235250702065617
18. Wilson-Welder JH, Torres MP, Kipper MJ, Mallapragada SK, Wannemuehler MJ, Narasimhan B, et al. Vaccine adjuvants: current challenges and future approaches. J Pharm Sci. 2009;98(4):1278-316. https://doi.org/10.1002/jps.21523
19. Lin P, Lin Y, Mai Z, Zheng Y, Zheng J, Zhou Z, et al. Targeting cancer with precision: strategical insights into TCR-engineered T cell therapies. Theranostics. 2025;15(1):300-323. https://doi.org/10.7150/thno.104594
Downloads
Published
Issue
Section
License
Copyright (c) 2026 Mubashra Inam, Kiran Rehman, Rabiya Atta (Author)

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.





