Evaluating the Antibiotic therapy in diabetic patients in diverse clinical settings
Keywords:
Diabetic Foot Infection, Antimicrobial Resistance, Resistance Burden Index, Gram-Negative Pathogens, Therapeutic StratificationAbstract
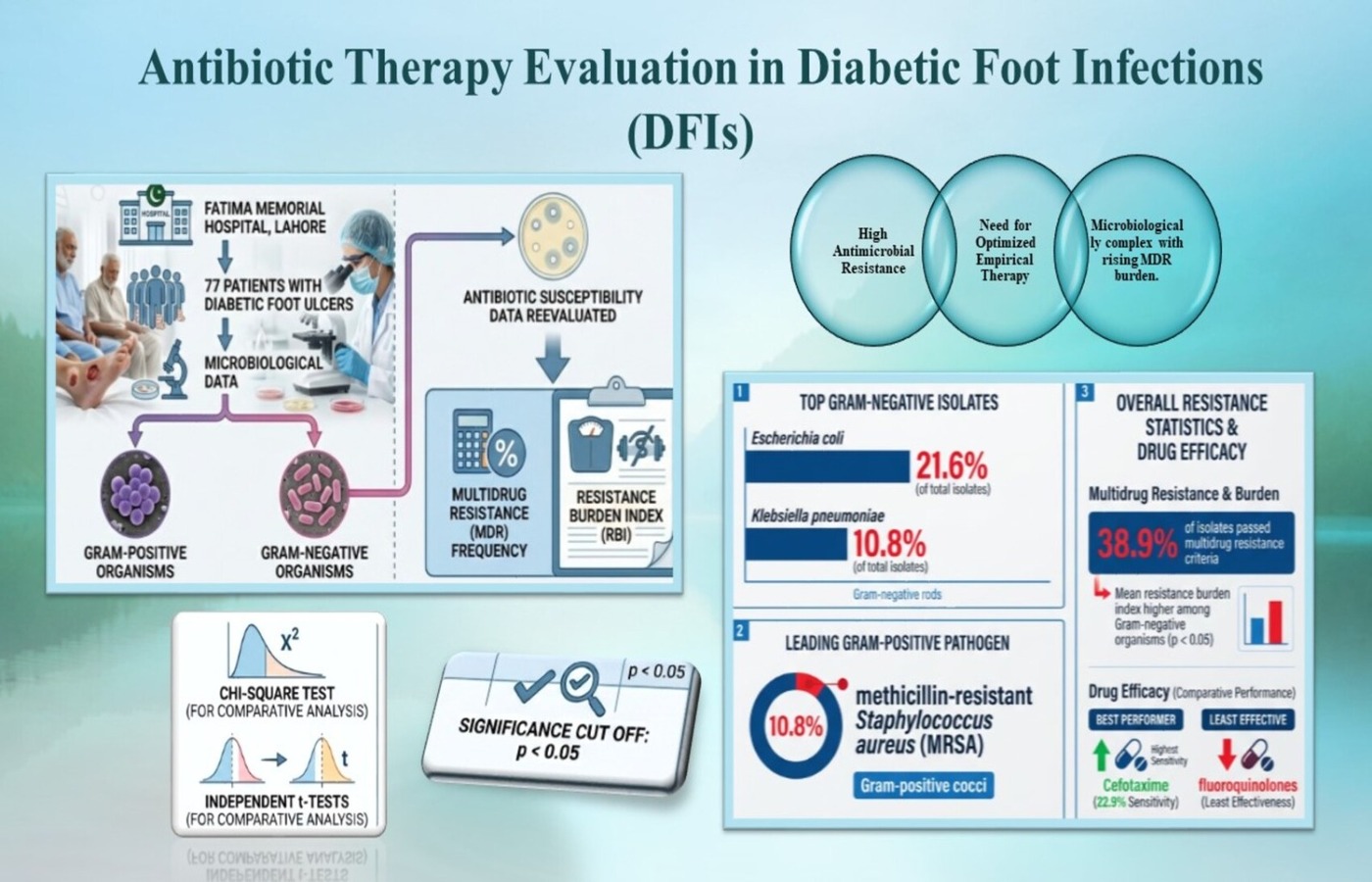
Background: Diabetic foot infections (DFIs) are considered a complicated combination of microbial pathogenicity, dysfunction of metabolic processes in the hosts, and response to therapy. The secondary analysis sought to reevaluate microbial distribution in DFIs based on resistance-based measures to direct optimal empirical therapy. Methods: The secondary evaluation of analyses was conducted on microbiological data of 77 patients with diabetic foot ulcers and getting treatment at the Fatima Memorial Hospital in Lahore, Pakistan. The organisms were categorized as Gram-negative or Gram-positive and antibiotic susceptibility data were reevaluated to calculate multidrug resistance (MDR) frequency and a resistance burden index (RBI). Chi-square and independent t-tests were used to support descriptive statistics with comparative analysis. The significance cut off of p was < 0.05. Results: Escherichia coli (21.6%) and Klebsiella pneumoniae (10.8%) were the most common Gram-negative (≥60%) and methicillin-resistant Staphylococcus aureus (MRSA) was of the most common Gram-positive pathogen (10.8%). Overall, 38.9% of the isolates passed multidrug resistance criteria. Mean resistance burden index was higher among Gram-negative organisms as opposed to Gram-positive isolates (p < 0.05). The highest sensitivity score (22.9%) was observed for Cefotaxime followed by imipenem and colistin, whereas fluoroquinolones had least effectiveness. Resistant burden was not statistically significantly related to any of the patient comorbidities (hypertension, obesity; p > 0.05). Conclusion: Quantitative resistance profiling serves the purpose of supporting the necessity of locally-constrained empirical regimens and endorsing cefotaxime-based strategies as well as reinforcing the imperative to practice antimicrobial stewardship.
References
1. Maity S, Leton N, Nayak N, Jha A, Anand N, Thompson K, et al. A systematic review of diabetic foot infections: pathogenesis, diagnosis, and management strategies. Front Clin Diabetes Healthc. 2024 Aug 6;5:1393309. https://doi.org/10.3389/fcdhc.2024.1393309
2. Hurlow JJ, Humphreys GJ, Bowling FL, McBain AJ. Diabetic foot infection: a critical complication. Int Wound J. 2018 Oct;15(5):814–821. https://doi.org/10.1111/iwj.12932
3. Hossain MJ, Al-Mamun M, Islam MR. Diabetes mellitus, the fastest growing global public health concern: early detection should be focused. Health Sci Rep. 2024 Mar;7(3):e2004. https://doi.org/10.1002/hsr2.2004
4. Cortes-Penfield NW, Armstrong DG, Brennan MB, Fayfman M, Ryder JH, Tan TW, et al. Evaluation and management of diabetes-related foot infections. Clin Infect Dis. 2023 Aug 1;77(3):e1–e3. https://doi.org/10.1093/cid/ciad255
5. Złoch M, Maślak E, Kupczyk W, Pomastowski P. Multi-instrumental analysis toward exploring the diabetic foot infection microbiota. Curr Microbiol. 2023 Aug;80(8):271. https://doi.org/10.1007/s00284-023-03384-z
6. Xie H, Chen Z, Wu G, Wei P, Gong T, Chen S, et al. Application of metagenomic next-generation sequencing to describe the microbial characteristics of diabetic foot ulcers at a tertiary medical center in South China. BMC Endocr Disord. 2025 Jan 24;25(1):18. https://doi.org/10.1186/s12902-025-01837-z
7. Bassetti M, Vena A, Labate L, Giacobbe DR. Empirical antibiotic therapy for difficult-to-treat Gram-negative infections: when, how, and how long? Curr Opin Infect Dis. 2022 Dec;35(6):568–574. https://doi.org/10.1097/QCO.0000000000000884
8. Lim L, Kassym L, Kussainova A, Aubakirova B, Semenova Y. Optimizing antibiotic stewardship and reducing antimicrobial resistance in Central Asia: a study protocol for evidence-based practice and policy. PLoS One. 2025 Jan 16;20(1):e0307784. https://doi.org/10.1371/journal.pone.0307784
9. Qu YD, Ou SJ, Zhang W, Li JX, Xia CL, Yang Y, et al. Microbiological profile of diabetic foot infections in China and worldwide: a 20-year systematic review. Front Endocrinol (Lausanne). 2024 Jun 28;15:1368046. https://doi.org/10.3389/fendo.2024.1368046
10. Huttenhower C, Finn RD, McHardy AC. Challenges and opportunities in sharing microbiome data and analyses. Nat Microbiol. 2023 Nov;8(11):1960–1970. https://doi.org/10.1038/s41564-023-01484-x
11. Sullivan KM, Dean A, Soe MM. On academics: OpenEpi: a web-based epidemiologic and statistical calculator for public health. Public Health Rep. 2009 May;124(3):471–474. https://doi.org/10.1177/003335490912400320
12. Dickson MC, Skrepnek GH. Hospitalization and health resource utilization in emergency department cases of diabetic foot infections in the United States from 2012 to 2021: a nationally representative analysis. J Clin Med. 2024 Sep 10;13(18):5361. https://doi.org/10.3390/jcm13185361
13. Ciarambino T, Crispino P, Leto G, Mastrolorenzo E, Para O, Giordano M. Influence of gender in diabetes mellitus and its complication. Int J Mol Sci. 2022 Aug 9;23(16):8850. https://doi.org/10.3390/ijms23168850
14. Ray A, Bonorden MJ, Pandit R, Nkhata KJ, Bishayee A. Infections and immunity: associations with obesity and related metabolic disorders. J Pathol Transl Med. 2023 Jan;57(1):28–42. https://doi.org/10.4132/jptm.2022.11.14
15. Zhang X, Tan L, Ouyang P, Ma H, Peng J, Shi T, et al. Distribution and antibiotic resistance of Gram-positive bacteria isolated from a tertiary-care hospital in southern China: an 8-year retrospective study. Front Microbiol. 2023 Sep 28;14:1220363. https://doi.org/10.3389/fmicb.2023.1220363
16. Gondane AA, Pawar DB. Activity of cefotaxime versus ceftriaxone against pathogens isolated from various systemic infections: a prospective multicenter comparative in vitro study. J Lab Physicians. 2023 Aug 16. https://doi.org/10.1055/s-0043-1772564
17. Jalil MB, Al Atbee MY. Prevalence of multidrug-resistant Escherichia coli and Klebsiella pneumoniae isolated from urinary tract infections. J Clin Lab Anal. 2022 Sep;36(9):e24619. https://doi.org/10.1002/jcla.24619
18. Bayaba S, Founou RC, Tchouangueu FT, Dimani BD, Mafo LD, Nkengkana OA, et al. High prevalence of multidrug-resistant and extended-spectrum β-lactamase–producing Escherichia coli and Klebsiella pneumoniae from urinary tract infections in Cameroon. BMC Infect Dis. 2025 Jan 24;25(1):115. https://doi.org/10.1186/s12879-025-10483-8
19. Hasmukharay K, Ngoi ST, Saedon NI, Tan KM, Khor HM, Chin AV, et al. Evaluation of methicillin-resistant Staphylococcus aureus bacteremia in older patients at a tertiary teaching hospital in Malaysia. BMC Infect Dis. 2023 Apr 18;23(1):241. https://doi.org/10.1186/s12879-023-08206-y
20. Edlund C, Ternhag A, Ståhlgren GS, Edquist P, Balkhed ÅÖ, Athlin S, et al. Clinical and microbiological efficacy of temocillin versus cefotaxime in adults with febrile urinary tract infection: a randomized multicenter clinical trial. Lancet Infect Dis. 2022 Mar;22(3):390–400. https://doi.org/10.1016/S1473-3099(21)00407-2
21. Díaz-Brochero C, Valderrama-Rios MC, Nocua-Báez LC, Cortés JA. First-generation cephalosporins for complicated upper urinary tract infection in adults: a systematic review. Int J Infect Dis. 2022 Mar;116:403–410. https://doi.org/10.1016/j.ijid.2021.12.363
22. Ali FA, Al-Daood AA, Ibrahim GS, Abdulla CA, Assad HM, Muhammed DW. Emergence of Raoultella ornithinolytica producing beta-lactamase enzyme in clinical specimens from Erbil City. South Asian J Res Microbiol. 2023 Jan 15;15(1):9–19. https://doi.org/10.9734/sajrm/2023/v15i1277
23. Cohen SP, Wang EJ, Doshi TL, Vase L, Cawcutt KA, Tontisirin N. Chronic pain and infection: mechanisms, causes, conditions, treatments, and controversies. BMJ Med. 2022 Mar 31;1(1):e000108. https://doi.org/10.1136/bmjmed-2021-000108
24. Russell CD, Lone NI, Baillie JK. Comorbidities, multimorbidity and COVID-19. Nat Med. 2023 Feb;29(2):334–343. https://doi.org/10.1038/s41591-022-02156-9
25. Nieuwland AJ, Waibel FW, Flury A, Lisy M, Berli MC, Lipsky BA, et al. Initial antibiotic therapy for postoperative moderate or severe diabetic foot infections: broad versus narrow spectrum, empirical versus targeted. Diabetes Obes Metab. 2023 Nov;25(11):3290–3297. https://doi.org/10.1111/dom.15228
Downloads
Published
Issue
Section
License
Copyright (c) 2025 Muhammad Junaid, Imran Sadiq (Author)

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.





