Perioperative Patient Safety: Are We Doing Enough in Resource-Limited Settings?
Keywords:
Patient safety, Perioperative care, Surgery, Anesthesia, Health Resources, Developing CountriesAbstract
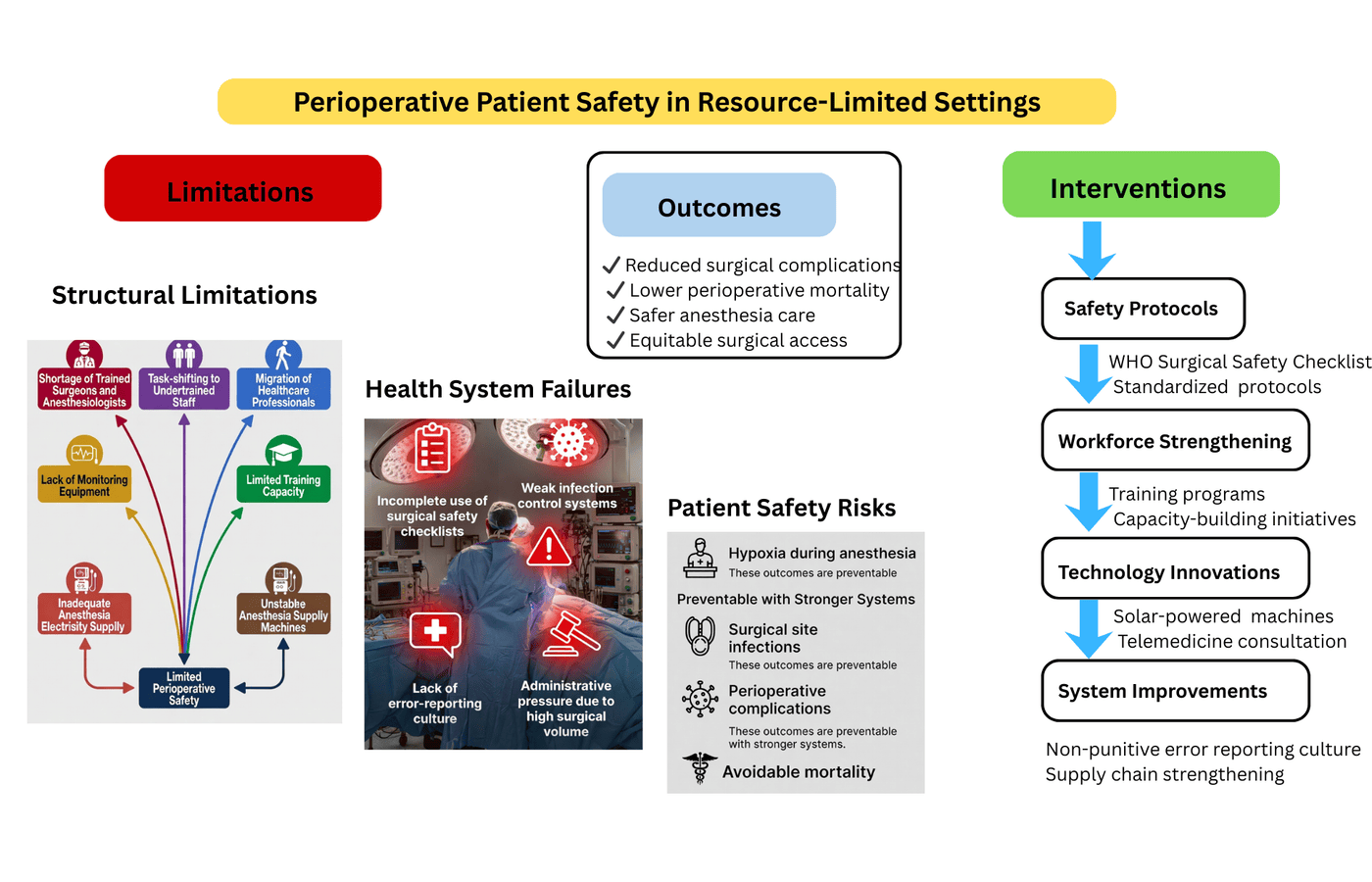
The perioperative safety is a core issue in surgery and anesthesia, but resources-constrained environments face a number of difficulties to ensure perioperative safety. The lack of skilled specialists, poor infrastructure, and inadequate access to monitoring and medications contribute extensively to the risk that could be prevented in patients. Although international checklists and safety guidelines are available, their application is frequently hampered by structural and personnel inadequacy. The costs and cultural restrictions also complicate the application of safe practices, especially to vulnerable communities in rural and low-income neighborhoods. Although the use of innovative solutions and multi-national partnerships has proven to be effective, the ongoing discrepancy between global guidelines and domestic realities has continued to undermine patient outcomes.
References
1. Amrita A, Kumari J, Sinha A, Singh A, Goel N, Poonam P, et al. Role of the WHO Surgical Safety Checklist in Reducing Morbidity and Mortality Among Obstetrics and Gynecology Patients Undergoing Surgery: A Prospective Comparative Study. Cureus. 2024 May;16(5):e60775. https://doi.org/10.7759/cureus.60775
2. Hinson C, Kilpatrick C, Rasa K, Ren J, Nthumba P, Sawyer R, et al. Global surgery is stronger when infection prevention and control is incorporated: a commentary and review of the surgical infection landscape. BMC Surg. 2024 Dec 20;24(1):397. https://doi.org/10.1186/s12893-024-02695-7
3. van Duinen AJ, Gyedu A. Task Shifting and Task Sharing to Strengthen the Surgical Workforce in Sub-Saharan Africa: A Systematic Review of the Existing Literature. World J Surg. 2023 Dec;47(12):3081–3082. https://doi.org/10.1007/s00268-023-07228-6
4. Dore MA, Torabizadeh C, Keshtkaran Z. Threats to operating room personnel’s occupational safety and health: a qualitative study. Anaesth Pain Intensive Care. 2022 Apr 6;26(3):368–381. https://doi.org/10.35975/apic.v26i3.1912
5. Iqbal M, Clement-Pervaiz MV, Ansari MJ, Pervaiz S, Sheikh S, Katpar S, et al. Proceedings of the 1st Liaquat University of Medical & Health Sciences (LUMHS) International Medical Research Conference. Eur J Med Res. 2017;22(Suppl 1):53. https://doi.org/10.1186/s40001-017-0296-3
6. Amin N, Mukherjee D, Sanapala V. Addressing anesthesia equipment issues: A step towards enhanced patient safety. J Anaesthesiol Clin Pharmacol. 2025 Apr–Jun;41(2):363–364. https://doi.org/10.4103/joacp.joacp_33_24
7. Qaiser S, Noman M, Khan MS, Ahmed UW, Arif A. The Role of WHO Surgical Checklists in Reducing Postoperative Adverse Outcomes: A Systematic Review. Cureus. 2024 Oct;16(10):e70923. https://doi.org/10.7759/cureus.70923
8. Aschbrenner KA, Walsh-Bailey C, Brown MC, Khan T, Baggett TP, Jones SMW, et al. Practical considerations for engaging staff in resource-constrained healthcare settings in implementation research: A qualitative focus group and consensus building study. J Clin Transl Sci. 2025 Mar 26;9(1):e65. https://doi.org/10.1017/cts.2025.29
9. Samad L, Ashraf MN, Mohammad AA, Fatima I, Fowler Z, Albutt K, et al. Access and Financial Burden for Patients Seeking Essential Surgical Care in Pakistan. Ann Glob Health. 2022 Dec 20;88(1):107. https://doi.org/10.5334/aogh.3784
10. Puja SS, Neha NN, Alif OR, Sultan TJ, Husna MdGZA, Jahan I, et al. Exploring the barriers to feminine healthcare access among marginalized women in Bangladesh and facilitating access through a voice bot. Heliyon. 2024 Jul 30;10(14):e33927. https://doi.org/10.1016/j.heliyon.2024.e33927
11. Mulugeta H, Zemedkun A, Mergia G, Abate SM, Gebremariam M, Jemal B, et al. Perioperative capacity and contextual challenges in teaching hospitals of southern Ethiopia: explanatory sequential mixed-methods research. Perioper Med. 2024 Jun 22;13:61. https://doi.org/10.1186/s13741-024-00423-6
12. Yusof ANM, Razali HYH. Moving Away from the Blame Culture: The Way Forward to Manage Medical Errors. Malays J Med Sci. 2024 Dec;31(6):126–132. https://doi.org/10.21315/mjms2024.31.6.10
13. Pai DR, Kumar VH, Sobana R. Perioperative crisis resource management simulation training in anaesthesia. Indian J Anaesth. 2024 Jan;68(1):36–44. https://doi.org/10.4103/ija.ija_1151_23
14. Seger C, Cannesson M. Recent advances in the technology of anesthesia. F1000Research. 2020 May 18;9:F1000 Faculty Rev-375. https://doi.org/10.12688/f1000research.24059.1
15. Rajabi M, Ebrahimi P, Aryankhesal A. Collaboration between the government and nongovernmental organizations in providing health-care services: A systematic review of challenges. J Educ Health Promot. 2021 Jun 30;10:242. https://doi.org/10.4103/jehp.jehp_1312_20
16. Calderwood MS, Anderson DJ, Bratzler DW, Dellinger EP, Garcia-Houchins S, Maragakis LL, et al. Strategies to prevent surgical site infections in acute-care hospitals: 2022 Update. Infect Control Hosp Epidemiol. 2023 May;44(5):695–720. https://doi.org/10.1017/ice.2023.67
Downloads
Published
Issue
Section
License
Copyright (c) 2026 Tayyaba Rafiq, Rummana Aqeel (Author)

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.





