Thyroid Hormone Dysregulation and Ovulatory Pathogenesis in Women: A Systematic Review and Meta-Analysis of Endocrine and Reproductive Biomarkers
Keywords:
Polycystic Ovary Syndrome, Thyroid Hormones, Thyrotropin, Triiodothyronine, Thyroxine, Ovulation Disorders, Infertility, Meta-AnalysisAbstract
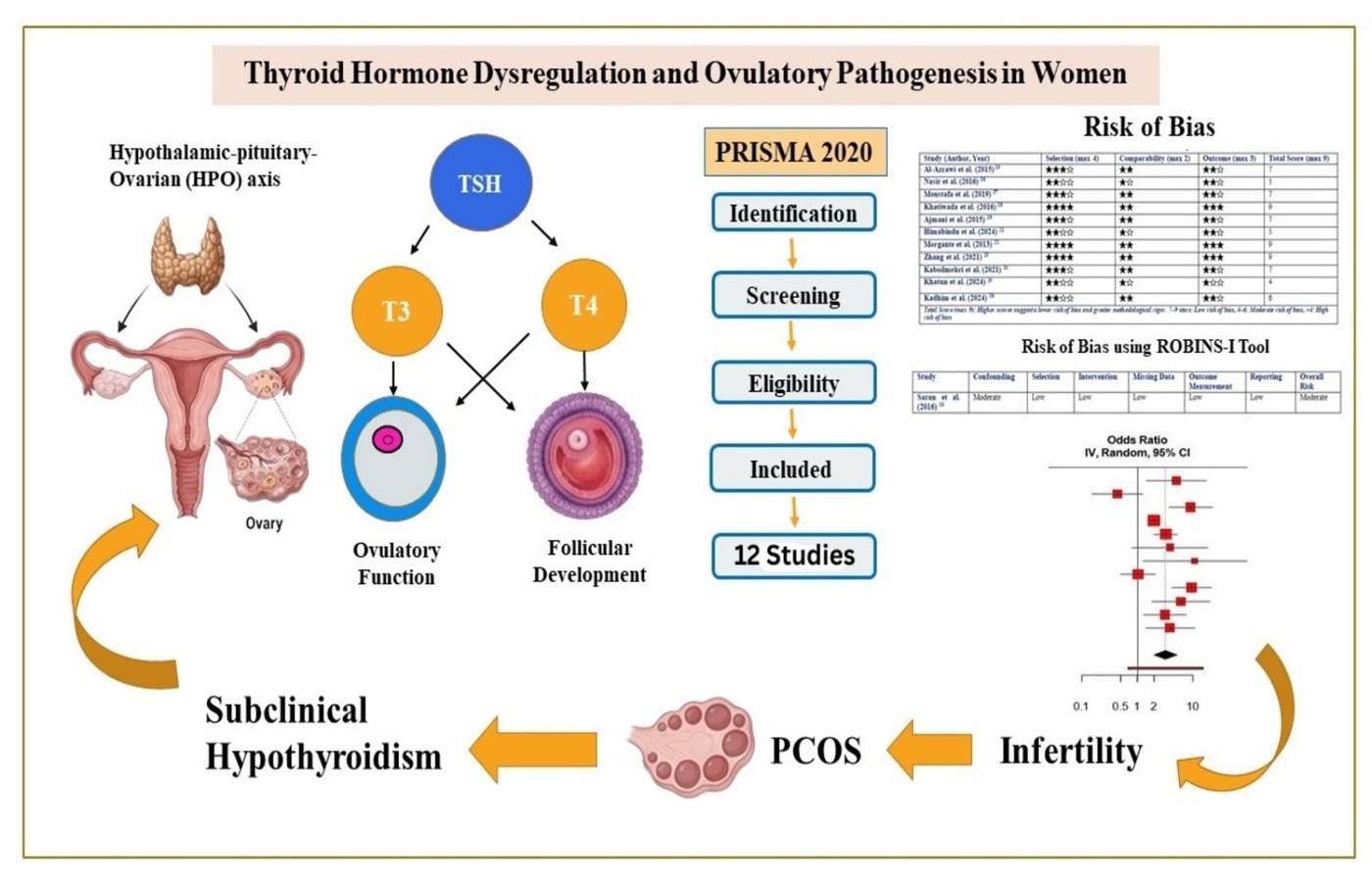
Background: Thyroid hormones play a major role in the maintenance of the hypothalamic-pituitary-ovarian axis and any form of imbalance may significantly impact on reproductive physiology. This meta-analysis and systematic review study aims at establishing the linkage between thyroid dysfunction and ovulatory disturbances in relation to its implication on reproductive health and infertility treatment. Methods: The study followed PRISMA guidelines and articles published till 2024 were retrieved from PubMed, Scopus, Web of Science, and the Cochrane Library. Studies that examined the association between thyroid malfunctioning and ovulatory/menstrual abnormalities were included. Studies lacking quantitative data for thyroid or ovulatory disorders were excluded. Risk of bias was measured using Newcastle-Ottawa Scale, and the quality of evidence was determined through GRADE assessment. Meta-analysis was performed using MetaAnalysisOnline tool. Results: The findings indicated a positive correlation between thyroid dysfunction and ovulatory defects (pooled risk ratio 3.20, 95% CI: 2.00–5.13, p < 0.0001). The heterogeneity was moderate (I² = 74.9%, p < 0.0001) and sensitivity analysis supported the accuracy of the study results. Conclusion: Subclinical hypothyroidism was the most commonly implicated condition, especially in women with Polycystic Ovary Syndrome (PCOS), reduced ovarian reserve and unexplained infertility. Additional longitudinal studies with standardized assessment protocols of hormones are needed to resolve the causality and to develop optimal patient-specific treatment strategies.
References
1. Bendarska-Czerwińska A, Zmarzły N, Morawiec E, Panfil A, Brys K, Czarniecka J, et al. Endocrine disorders and fertility and pregnancy: An update. Front Endocrinol. 2023;13:970439. https://doi.org/10.3389/fendo.2022.970439
2. Brown EDL, Obeng-Gyasi B, Hall JE, Shekhar S. The thyroid hormone axis and female reproduction. Int J Mol Sci. 2023;24(12):9815. https://doi.org/10.3390/ijms24129815
3. Zhu Y, Wu X, Zhou R, Sie O, Niu Z, Wang F, et al. Hypothalamic-pituitary-end-organ axes: Hormone function in female patients with major depressive disorder. Neurosci Bull. 2021;37(8):1176–1187. https://doi.org/10.1007/s12264-021-00689-6
4. Palomba S, Colombo C, Busnelli A, Caserta D, Vitale G. Polycystic ovary syndrome and thyroid disorder: A comprehensive narrative review of the literature. Front Endocrinol. 2023;14:1251866. https://doi.org/10.3389/fendo.2023.1251866
5. Fan H, Ren Q, Sheng Z, Deng G, Li L. The role of the thyroid in polycystic ovary syndrome. Front Endocrinol. 2023;14:1242050. https://doi.org/10.3389/fendo.2023.1242050
6. Saei Ghare Naz M, Rostami Dovom M, Ramezani Tehrani F. The menstrual disturbances in endocrine disorders: A narrative review. Int J Endocrinol Metab. 2020;18(4):e106694. https://doi.org/10.5812/ijem.106694
7. Krassas GE, Markou KB. The impact of thyroid diseases starting from birth on reproductive function. Hormones (Athens). 2019;18(4):365–381. https://doi.org/10.1007/s42000-019-00156-y
8. Wang R, Lv Y, Dou T, Yang Q, Yu C, Guan Q. Autoimmune thyroid disease and ovarian hypofunction: A review of literature. J Ovarian Res. 2024;17(1):125. https://doi.org/10.1186/s13048-024-01451-y
9. Emanuel RHK, Roberts J, Docherty PD, Lunt H, Campbell RE, Möller K. A review of the hormones involved in the endocrine dysfunctions of polycystic ovary syndrome and their interactions. Front Endocrinol. 2022;13:1017468. https://doi.org/10.3389/fendo.2022.1017468
10. Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. https://doi.org/10.1136/bmj.n71
11. Luchini C, Stubbs B, Solmi M, Veronese N. Assessing the quality of studies in meta-analyses: Advantages and limitations of the Newcastle–Ottawa Scale. World J Meta-Anal. 2017;5(4):80–84. https://doi.org/10.13105/wjma.v5.i4.80
12. Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, et al. ROBINS-I: A tool for assessing risk of bias in non-randomised studies of interventions. BMJ. 2016;355:i4919. https://doi.org/10.1136/bmj.i4919
13. Prasad M. Introduction to the GRADE tool for rating certainty in evidence and recommendations. Clin Epidemiol Glob Health. 2024;25:101484. https://doi.org/10.1016/j.cegh.2023.101484
14. Fekete JT, Győrffy B. MetaAnalysisOnline.com: Web-based tool for the rapid meta-analysis of clinical and epidemiological studies. J Med Internet Res. 2025;27:e64016. https://doi.org/10.2196/64016
15. Al-Azzawi OD, Al-Hadithy A, Amen SS. The effect of thyroid dysfunction on anti-mollurian hormone concentration in the infertile women at the fertile age. Int J Sci Nat. 2015 Jan;6(1):45–50. https://www.researchgate.net/publication/335777596
16. Nasir S, Khan MM, Ahmad S, Alam S, Ziaullah S. Role of thyroid dysfunction in infertile women with menstrual disturbances. Gomal J Med Sci. 2016;14(1). https://gjms.com.pk/index.php/journal/article/view/640
17. Moustafa MM, Jamal MY, Al-Janabi RD. Thyroid hormonal changes among women with polycystic ovarian syndrome in Baghdad–a case-control study. F1000Research. https://f1000research.com/articles/8-669
18. Khatiwada S, Gautam S, Kc R, Singh S, Shrestha S, Jha P, et al. Pattern of thyroid dysfunction in women with menstrual disorders. Ann Clin Chem Lab Med. 2016;2(1):3–6. https://doi.org/10.3126/acclm.v2i1.14195
19. Ajmani NS, Sarbhai V, Yadav N, Paul M, Ahmad A, Ajmani AK. Role of thyroid dysfunction in patients with menstrual disorders in a tertiary care center of walled city of Delhi. J Obstet Gynaecol India. 2016;66(2):115–119. https://doi.org/10.1007/s13224-014-0650-0
20. Saran S, Gupta BS, Philip R, Singh KS, Bende SA, Agroiya P, et al. Effect of hypothyroidism on female reproductive hormones. Indian J Endocrinol Metab. 2016;20(1):108. https://doi.org/10.4103/2230-8210.172245
21. Penumalla HH, G S, K P, Penumalla S, Kandimalla R. Hypothyroidism and its impact on menstrual irregularities in reproductive-age women: A comprehensive analysis at a tertiary care center. Cureus. 2024;16(6):e63158. https://doi.org/10.7759/cureus.63158
22. Morgante G, Musacchio MC, Orvieto R, Massaro MG, De Leo V. Alterations in thyroid function among different polycystic ovary syndrome phenotypes. Gynecol Endocrinol. 2013;29(11):967–969. https://doi.org/10.3109/09513590.2013.829445
23. Zhang Y, Wu W, Liu Y, Wang X, Guan Y, Jia L. Analysis of basal serum TSH, FT3, and FT4 levels based on age and sampling time in women with infertility. BMC Womens Health. 2021;21(1):317. https://doi.org/10.1186/s12905-021-01453-8
24. Kabodmehri R, Sharami SH, Sorouri ZZ, Gashti NG, Milani F, Chaypaz Z, et al. The relationship between thyroid function and ovarian reserve: A prospective cross-sectional study. Thyroid Res. 2021;14(1):22. https://doi.org/10.1186/s13044-021-00112-2
25. Khatun W, Kamal AHM, Lina KSN. Thyroid dysfunctions in patients with menstrual disturbances. TAJ J Teach Assoc. 2024;37(1):41–48. https://doi.org/10.70818/taj.v37i1.0165
26. Mohammad AK, Al-Qarawy AKM, Al-Obaidi ZME. A study of the relation between hypothyroidism and serum anti-Müllerian hormone in infertile women. Med Forum Mon. 2024;35(8). https://doi.org/10.60110/medforum.350802
27. Serin AN, Birge Ö, Uysal A, Görar S, Tekeli F. Hashimoto’s thyroiditis worsens ovarian reserve in polycystic ovary syndrome patients based on anti-Müllerian hormone levels. BMC Endocr Disord. 2021;21(1):44. https://doi.org/10.1186/s12902-021-00706-9
28. Bucci I, Giuliani C, Di Dalmazi G, Formoso G, Napolitano G. Thyroid autoimmunity in female infertility and assisted reproductive technology outcomes. Front Endocrinol. 2022;13:768363. https://doi.org/10.3389/fendo.2022.768363
29. Dhillon-Smith RK, Tobias A, Smith PP, Middleton LJ, Sunner KK, Baker K, et al. Prevalence of thyroid dysfunction and autoimmunity in women with history of miscarriage or subfertility. J Clin Endocrinol Metab. 2020;105(8):2667–2677. https://doi.org/10.1210/clinem/dgaa302
30. Kalra S, Aggarwal S, Khandelwal D. Thyroid dysfunction and dysmetabolic syndrome: The need for enhanced thyrovigilance strategies. Int J Endocrinol. 2021;2021:9641846. https://doi.org/10.1155/2021/9641846
31. Rao M, Wang H, Zhao S, Liu J, Wen Y, Wu Z, et al. Subclinical hypothyroidism is associated with lower ovarian reserve in women aged 35 years or older. Thyroid. 2020;30(1):95–105. https://doi.org/10.1089/thy.2019.0031
32. Ünsal İ, Hepşen S, Akhanlı P, Calapkulu M, Sencar ME, Yalçındağ A, et al. Evaluation of serum anti-Müllerian hormone levels in women with Hashimoto thyroiditis of reproductive age. Turk J Med Sci. 2021;51(2):716–721. https://doi.org/10.3906/sag-2012-177
33. Gawron I, Baran R, Jach R. Ovarian function measures in normogonadotropic anovulation and subclinical thyroid dysfunction: A prospective cohort study. Endocrine. 2025;88(1):330–347. https://doi.org/10.1007/s12020-024-04151-1
34. Poppe K, Bisschop P, Fugazzola L, Minziori G, Unuane D, Weghofer A. European Thyroid Association guideline on thyroid disorders prior to and during assisted reproduction. Eur Thyroid J. 2021;10(1):1–18. https://doi.org/10.1159/000512790
35. Koyyada A, Orsu P. Role of hypothyroidism and associated pathways in pregnancy and infertility: Clinical insights. Tzu Chi Med J. 2020;32(4):312. https://doi.org/10.4103/tcmj.tcmj_255_19
36. Köhrle J, Frädrich C. Thyroid hormone system disrupting chemicals. Best Pract Res Clin Endocrinol Metab. 2021;35(5):101562. https://doi.org/10.1016/j.beem.2021.101562
37. Barbagallo F, Cannarella R, Condorelli RA, Cucinella L, Vignera S, Nappi R, et al. Thyroid diseases and female sexual dysfunctions. Sex Med Rev. 2024;12(3):321–333. https://doi.org/10.1093/sxmrev/qeae021
38. Fu J, Zhang G, Xu P, Guo R, Li J, Guan H, Li Y. Seasonal changes of thyroid function parameters in women of reproductive age between 2012 and 2018: A retrospective, observational, single-center study. Front Endocrinol (Lausanne). 2021;12:719225. https://doi.org/10.3389/fendo.2021.719225
39. Abood BH, Alhussaynei AJ. Effect of thyroid gland dysfunction on menstrual pattern among women of reproductive age. Int J Health Sci (Qassim). 2022;6(Suppl 9):566–575. https://doi.org/10.53730/ijhs.v6nS9.12234
40. Lipkin P, Monseur B, Mayo J, Moravek M, Nahata L, Amato P, Alvero R, Obedin-Maliver J. Reproductive endocrinologist and infertility specialists’ knowledge, skills, behaviors, and attitudes regarding the care for transgender and gender-diverse individuals. F&S Rep. 2023;4(2):213–223. https://doi.org/10.1016/j.xfre.2023.03.009
Downloads
Published
Issue
Section
License
Copyright (c) 2025 Nimra Asghar, Zuha Tariq, Minahil Tahir, Fatima Ali, Muhammad Akram, Ejaz Khan, Khaleeq Ullah (Author)

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.





