Global Floods and Public Health: Anticipating Outbreaks of Vector-Borne and Waterborne Diseases in Vulnerable Countries
Keywords:
Floods, Natural Disaster, Pakistan, Vector-borne diseases, Waterborne-diseasesAbstract
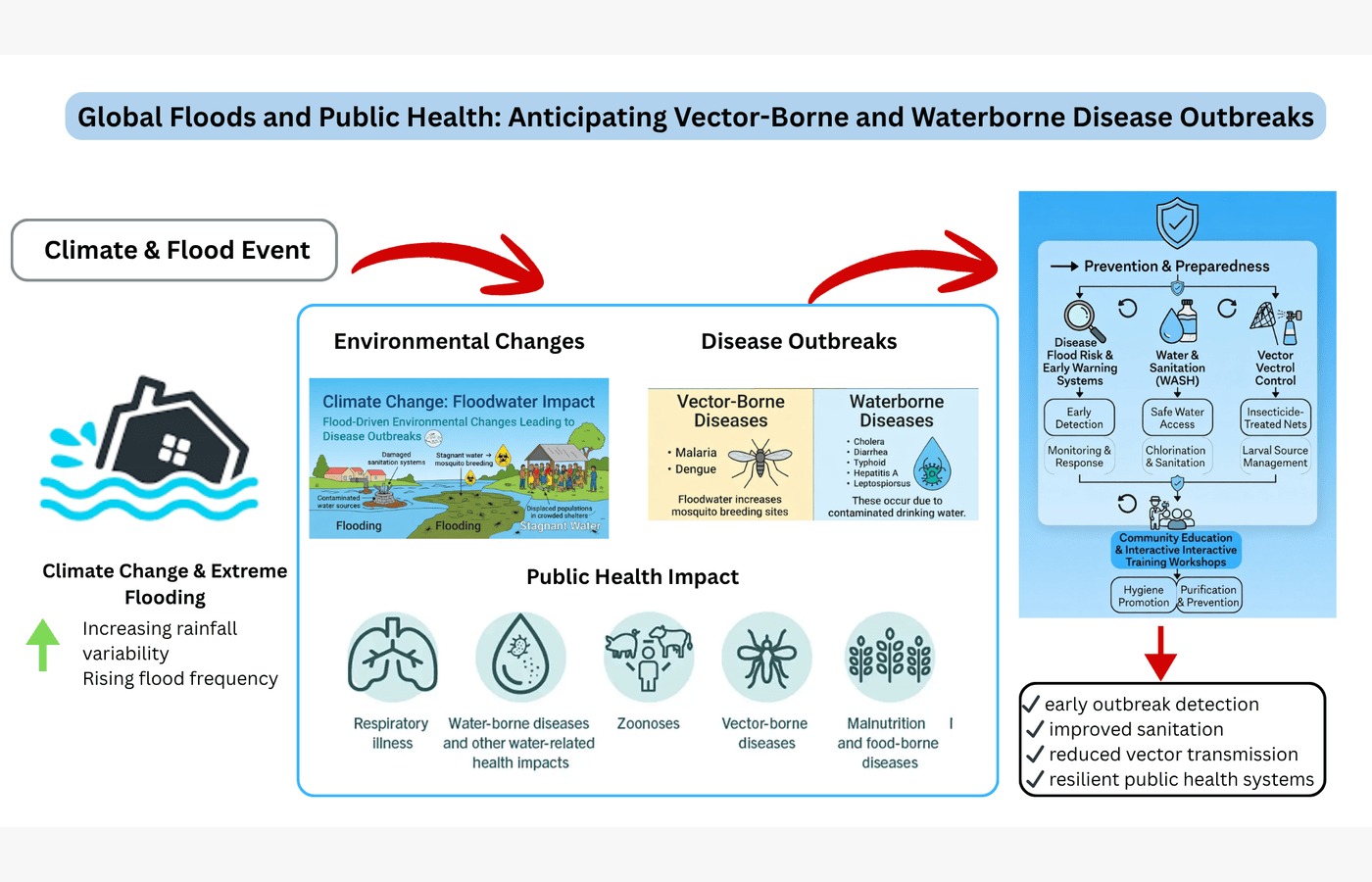
Floods create insidious epidemics within the public health that are usually discovered too late. Floods are not mere natural tragedies; they cause eruption of water borne diseases and virus carrying diseases 1. Unless we are able to plan and respond in time, the human cost of flooding will be far greater than drowned villages and forced families. The 2022 flood in Pakistan affected 33 million lives 2. The recent 2025 flood, which have yet to be actively recorded in literature, have alarmingly trends. Stagnant water provided the breeding grounds to the mosquitoes leading to the outbreaks of malaria and dengue 3. The contaminated water sources caused a large-scale eruption of diarrhea and cholera particularly among those children under the age of five 4. According to the World Health Organization (WHO), over 8 million people sought medical help in Pakistan in just a few months because of flood-related diseases 5. These figures are rather grim: as the floods could not be stopped, and only time can tell the damage it will cause to public health.
Pakistan is not the lone sufferer of flood associated miseries. Other countries have also experienced similar catastrophes, such as the 2014 Southeastern Europe floods, the 2018 Kerala floods, in India, and the 2020 Yangtze River basin floods, in China 6. These disasters reveal that most nations are unprepared and that international cooperation is needed in efforts to save lives. In 1998, after extensive flooding in South Asia, a huge epidemic of cholera was witnessed in several countries with limited healthcare facilities due to the lack of water and sanitation 7. The message is simple: floods and epidemics cannot be separated because of the situation where water, sanitation infrastructure, and health systems are weak. This can be seen far beyond South Asia. In Sub-Saharan Africa, malaria is commonly fueled by recurrent floods 8. Mozambique has repeatedly faced malaria epidemics, alongside outbreaks of respiratory illnesses and diarrhea 9. Likewise, in Nigeria and Sudan, floodwater is usually contaminated, thereby triggering epidemics of cholera, leptospirosis, typhoid, and hepatitis A 10. Flooding increases the pre-existing deficits and transforms natural risks into long-term social health catastrophes.
Climate change worsens this problem every year. Floods are becoming common and adverse due to changes in temperature and the distribution of rain. The Intergovernmental Panel on Climate Change (IPCC) has warned that countries with fragile infrastructure and limited resources will bear the greatest impact of floods by the climate change 11. Moreover, disease epidemics do not follow geographical boundaries. The devastations of the floods in Pakistan, the cholera outbreak in Bangladesh and the malaria pandemic in Africa are lessons that apply across the board. Regardless of these evidences, during flood response planning there is a tendency that public health is a secondary concern. The first response of relief is usually centered on food distribution, shelter, and rebuilding of infrastructure. These priorities are necessary but often delay the urgent medical interventions. A cholera epidemic can roll back decades of child health advances; a malaria outbreak can bring whole neighborhoods to their knees; a diarrheal epidemic can wipe out malnourished communities. Unless addressed, the results of these health impacts may be even deadlier than the floods themselves 12.
Governments, humanitarian agencies, and international donors need to change their priorities in order to address this issue. Flood response needs to involve strong public health management, such as developing prompt disease surveillance systems in flood-prone regions to monitor the outbreak of malaria, dengue, cholera, and diarrhea 13. A delivery of safe drinking water, chlorine tablets, and temporary sanitation facilities to displaced people. By providing mosquito nets, insecticides, and other preventive strategies against the transmission of water-borne diseases 14. Educating communities about hygiene, water purification, and mosquito prevention 15. These measures are not optional rather a guide plan for flood recovery initiative. The well-being of the survivors is not just a will-have-it-fast, but the basics on which recovery relies 16. A society ravaged by disease is unable to resettle houses, reconstruct lives, and school its children.
Floods bring disasters that are more damaging to human lives than to the infrastructure in Pakistan, Bangladesh, and Mozambique. They create openings which allow diseases to spread, and enhance the pain while paralyze the healing. To deal with floods without laying stress on the health of the people is like fixing fences when the frame is broken. In case we are ready to lower the human price of floods, the forecasting and prevention of the public health crisis should be regarded as the primary priority. Only at that point can the communities in question really get back on their feet, not just in terms of roadways and bridges, but also lives, health, and dignity.
References
1. Acosta-España JD, Romero-Alvarez D, Luna C, Rodriguez-Morales AJ. Infectious disease outbreaks in the wake of natural flood disasters: global patterns and local implications. Infez Med. 2024 Dec;32(4):451–462. https://doi.org/10.53854/liim-3204-4
2. Qamer FM, Abbas S, Ahmad B, Hussain A, Salman A, Muhammad S, et al. A framework for multi-sensor satellite data to evaluate crop production losses: the case study of 2022 Pakistan floods. Sci Rep. 2023 Mar 14;13(1):4240. https://doi.org/10.1038/s41598-023-30347-y
3. Coalson JE, Anderson EJ, Santos EM, Madera Garcia V, Romine JK, Dominguez B, et al. The Complex Epidemiological Relationship between Flooding Events and Human Outbreaks of Mosquito-Borne Diseases: A Scoping Review. Environ Health Perspect. 2021 Sep;129(9):96002. https://doi.org/10.1289/EHP8887
Erratum: Environ Health Perspect. 2021 Dec;129(12):129001. https://doi.org/10.1289/EHP10706
4. Yirdaw G, Mekonen H, Assaye BT, Amare GA, Yenew C. Prevalence of acute diarrhea and its risk factors among under five children in flood affected Dasenech District, Southern Ethiopia: a cross-sectional study. Sci Rep. 2025 May 15;15(1):16980. https://doi.org/10.1038/s41598-025-02120-w
5. Bhutto S, Vighio K, Bhutto N, Alam S. Comprehensive analysis of health impacts arising from flood disasters: Evidence from Pakistan’s vulnerable regions. J Econ Manag Bus Adm. 2024 Dec 25;3(2):52–64. https://doi.org/10.59075/jemba.v3i2.501
6. Alcayna T, Rao VB, Lowe R. Identifying the climate sensitivity of infectious diseases: a conceptual framework. Lancet Planet Health. 2025 Aug 2;9:e101291. https://doi.org/10.1016/j.lanplh.2025.101291
7. Malikzai A, Qamar K, Shaeen SK, Malik UU, Rafique F. Cholera spike following monsoon floods in Pakistan: Challenges, efforts and recommendations. Int J Surg Open. 2023 Aug 1;57:100652. https://doi.org/10.1016/j.ijso.2023.100652
8. Salvador EC, Buddha N, Bhola A, Sinha SK, Kato M, Wijesinghe PR, et al. Health Emergency Risk Management in World Health Organization - South-East Asia Region during 2014–2023: synthesis of experiences. Lancet Reg Health Southeast Asia. 2023 Oct 29;18:100304. https://doi.org/10.1016/j.lansea.2023.100304
9. Kondo H, Seo N, Yasuda T, Hasizume M, Koido Y, Ninomiya N, et al. Post-flood—infectious diseases in Mozambique. Prehosp Disaster Med. 2002 Sep;17(3):126–133. https://doi.org/10.1017/S1049023X00000340
10. Davies GI, McIver L, Kim Y, Hashizume M, Iddings S, Chan V. Water-borne diseases and extreme weather events in Cambodia: review of impacts and implications of climate change. Int J Environ Res Public Health. 2014 Dec 23;12(1):191–213. https://doi.org/10.3390/ijerph12010191
11. Hunka N, Duncanson L, Armston J, Dubayah R, Healey SP, Santoro M, et al. Intergovernmental Panel on Climate Change (IPCC) Tier 1 forest biomass estimates from Earth Observation. Sci Data. 2024 Oct 14;11(1):1127. https://doi.org/10.1038/s41597-024-03930-9
12. Memon S, Bano U, Singha SP, Shahani MY, Shaikh P, Shahani SB, et al. Chromium restriction in the intrauterine environment and development of metabolic diseases in mice offspring. J Taibah Univ Med Sci. 2025;20(3):365–75. https://doi.org/10.1016/j.jtumed.2025.06.001
13. Ahmed SH, Shaikh TG, Waseem S, Zahid M, Mohamed Ahmed KAH, Irfan U, Hasibuzzaman MA. Water-related diseases following flooding in South Asian countries—a healthcare crisis. Eur J Clin Exp Med. 2024 Mar 30;22(1):232–242. https://doi.org/10.15584/ejcem.2024.1.29
14. Yazdi MS, Ardalan MA, Hosseini M, Yousefi Zoshk M, Hami Z, Heidari R, et al. Infectious Diarrhea Risks as a Public Health Emergency in Floods; a Systematic Review and Meta-Analysis. Arch Acad Emerg Med. 2024 May 5;12(1):e46. https://doi.org/10.22037/aaem.v12i1.2284
15. Nyawanda BO, Kariuki S, Khagayi S, Bigogo G, Danquah I, Munga S, et al. Forecasting malaria dynamics based on causal relations between control interventions, climatic factors, and disease incidence in western Kenya. J Glob Health. 2024 Oct 11;14:04208. https://doi.org/10.7189/jogh.14.04208
16. Sheerazi S, Awad SA, von Schreeb J. Use of mobile health units in natural disasters: a scoping review. BMC Health Serv Res. 2025 Mar 12;25(1):368. https://doi.org/10.1186/s12913-024-12067-9
17. De Wit S, Luseka E, Bradley D, Brown J, Bhagwan J, Evans B, et al. Water, sanitation and hygiene (WASH): the evolution of a global health and development sector. BMJ Glob Health. 2024 Oct 4;9(10):e015367. https://doi.org/10.1136/bmjgh-2024-015367
Downloads
Published
Issue
Section
License
Copyright (c) 2026 Babar Hayat (Author)

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.





