Beyond PD-1/PD-L1: TME-Targeted Therapies in the Era of Immunotherapy Resistance
Keywords:
Tumor Microenvironment, Immunotherapy, Programmed Cell Death-1 Receptor, T-Lymphocytes, Myeloid-Derived Suppressor Cells, Extracellular MatrixAbstract
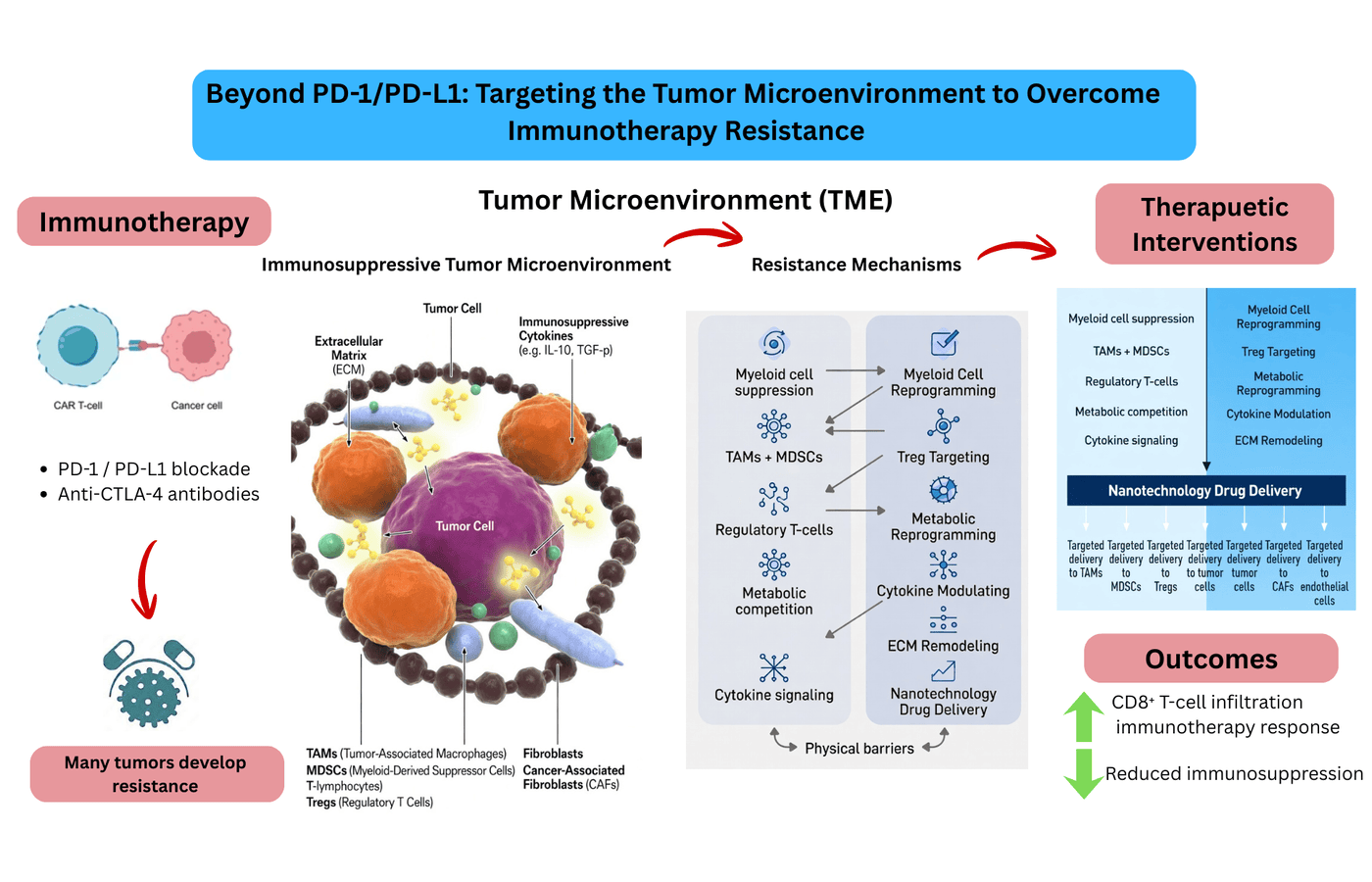
Blockade of PD-1/PD-L1 axis has revolutionized the cancer treatment, but clinical responses are often compromised by acquired resistance. Recent data suggested that tumor microenvironment (TME) is a key contributor of immunotherapy failure due to its ability to suppress immune reactions, place metabolic limitations, alter cytokine signaling, and extracellular matrix remodeling. This editorial identifies some of the TME-mediated resistance mechanisms and explains how new therapeutic approaches could be transformed beyond PD-1/PD-L1. Strategies such as myeloid cell reprogramming, regulatory T-cell regulation, metabolic therapy, neutralization of cytokines, targeting of extracellular matrix, and nanotechnology-mediated drug delivery are discussed as new promising perspectives in the context of immunotherapy resistance to restore antitumor immunity.
References
1. Goenka A, Shiravand Y, Khodadadi F, Kashani SMA, Hosseini-Fard SR, Hosseini S, et al. Immune checkpoint inhibitors in cancer therapy. Curr Oncol. 2022;29(5):3044–60. https://doi.org/10.3390/curroncol29050247
2. Lee H, Kim B, Park J, Park S, Yoo G, Yum S, et al. Cancer stem cells: landscape, challenges and emerging therapeutic innovations. Signal Transduct Target Ther. 2025;10:248. https://doi.org/10.1038/s41392-025-02360-2
3. Chen X, Feng L, Huang Y, Wu Y, Xie N. Mechanisms and strategies to overcome PD-1/PD-L1 blockade resistance in triple-negative breast cancer. Cancers (Basel). 2022;15(1):104. https://doi.org/10.3390/cancers15010104
4. Haist M, Stege H, Grabbe S, Bros M. The functional crosstalk between myeloid-derived suppressor cells and regulatory T cells within the immunosuppressive tumor microenvironment. Cancers (Basel). 2021;13(2):210. https://doi.org/10.3390/cancers13020210
5. Liu Y, Liang J, Zhang Y, Guo Q. Drug resistance and tumor immune microenvironment: an overview of current understandings. Int J Oncol. 2024;65:96. https://doi.org/10.3892/ijo.2024.5684
6. Deng J, Fleming JB. Inflammation and myeloid cells in cancer progression and metastasis. Front Cell Dev Biol. 2022;9:759691. https://doi.org/10.3389/fcell.2021.759691
7. Ai L, Chen J, Yan H, He Q, Luo P, Xu Z, et al. Research status and outlook of PD-1/PD-L1 inhibitors for cancer therapy. Drug Des Devel Ther. 2020;14:3625–49. https://doi.org/10.2147/DDDT.S267433
8. Sakaguchi S, Kawakami R, Mikami N. Treg-based immunotherapy for antigen-specific immune suppression and stable tolerance induction: a perspective. Immunotherapy Advances. 2023 Jan 1;3(1):ltad007. https://doi.org/10.1093/immadv/ltad007
9. Peng Y, Fu Y, Liu H, Zhao S, Deng H, Jiang X, et al. Non‐IL‐2‐blocking anti‐CD25 antibody inhibits tumor growth by depleting Tregs and has synergistic effects with anti‐CTLA‐4 therapy. International Journal of Cancer. 2024 Apr 1;154(7):1285-97. https://doi.org/10.1002/ijc.34823
10. Zhang A, Fan T, Liu Y, Yu G, Li C, Jiang Z. Regulatory T cells in immune checkpoint blockade antitumor therapy. Mol Cancer. 2024;23(1):251. https://doi.org/10.1186/s12943-024-02156-y
11. J Nankani GR, Memon S, Shaikh P, Farukh S. Non-small cell lung cancer: news from immunotherapy. J Lung Pulm Respir Res. 2022;9(1):8-10. https://doi.org/10.15406/jlprr.2022.09.00271
12. Arner EN, Rathmell JC. Metabolic programming and immune suppression in the tumor microenvironment. Cancer Cell. 2023;41(3):421–33. https://doi.org/10.1016/j.ccell.2023.01.009
13. Qazi N, Memon S, Memon F, Goswami P, Sirhandi BR, Goswami B. Antioxidant and hepato-protective effects of ginger in comparison with atorvastatin in hyperlipidemic albino mice. JMMC. 2024;15(1):21-6. https://doi.org/10.62118/jmmc.v15i1.464
14. Habibi MA, Nejati N, Najafi MB, Khodadadiyan A, Dashti M, Lorestani P, et al. Enhancing T cell infiltration in glioblastoma: challenges and therapeutic strategies. Cancer Treat Res Commun. 2025;45:100999. https://doi.org/10.1016/j.ctarc.2025.100999
15. Prakash J, Shaked Y. The interplay between extracellular matrix remodeling and cancer therapeutics. Cancer Discov. 2024;14(7):1375–88. https://doi.org/10.1158/2159-8290.CD-24-0002
16. Feng J, He D, Chen J, Li M, Luo J, Han Y, et al. Cell membrane biomimetic nanoplatforms: a new strategy for immune escape and precision targeted therapy. Mater Today Bio. 2025;35:102343. https://doi.org/10.1016/j.mtbio.2025.102343
17. Oroojalian F, Beygi M, Baradaran B, Mokhtarzadeh A, Shahbazi MA. Immune cell membrane‐coated biomimetic nanoparticles for targeted cancer therapy. Small. 2021 Mar;17(12):2006484. https://doi.org/10.1002/smll.202006484
18. Shi X, Wang X, Yao W, Shi D, Shao X, Lu Z, et al. Mechanism insights and therapeutic intervention of tumor metastasis: latest developments and perspectives. Signal Transduct Target Ther. 2024;9:192. https://doi.org/10.1038/s41392-024-01885-2
19. Fu R, Qi R, Xiong H, Lei X, Jiang Y, He J, et al. Combination therapy with oncolytic virus and T cells or mRNA vaccine amplifies antitumor effects. Signal Transduct Target Ther. 2024;9:118. https://doi.org/10.1038/s41392-024-01824-1
Downloads
Published
Issue
Section
License
Copyright (c) 2026 Asma Khawaja, Abdul Mannan Jehangir (Author)

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.





